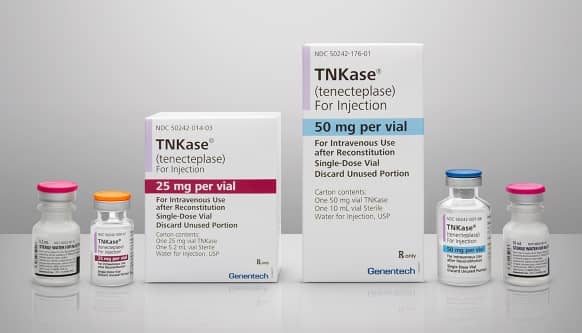
AVAILABLE IN 25-mg and 50-mg VIALS1

AVAILABLE IN 25-mg and 50-mg VIALS1

Have questions? Call 1-844-4-LYTICS (1-844-459-8427)
IV=intravenous.
Integrating TNKase into practice
Could the single 5-second IV bolus administration of TNKase benefit your patients with acute ischemic stroke?
TNKase® (tenecteplase) is a tissue plasminogen activator (tPA) indicated for the treatment of acute ischemic stroke (AIS) in adults. Learn more about the importance of timely treatment within 3 hours of symptom onset and the urgency to treat acute ischemic stroke.
TNKase is approved in 25-mg and 50-mg vials. Delivered as a single 5-second IV bolus in a hospital setting, TNKase® dosing is determined based on patient weight.
TNKase should not be used when contraindicated due to an increased risk of bleeding. It has warnings associated with bleeding, Hypersensitivity, Thromboembolism, Cholesterol Embolization and Arrhythmias. The most common adverse reaction is bleeding.
-
-
TNKase Prescribing Information. South San Francisco, CA. Genentech, Inc.
TNKase Prescribing Information. South San Francisco, CA. Genentech, Inc.
-
Tsao CW, Aday AW, Almarzooq ZI, et al. Heart disease and stroke statistics—2023 update: a report from the American Heart Association. Circulation. 2023;147(8):e93-e621. doi:10.1161/CIR.0000000000001123
Tsao CW, Aday AW, Almarzooq ZI, et al. Heart disease and stroke statistics—2023 update: a report from the American Heart Association. Circulation. 2023;147(8):e93-e621. doi:10.1161/CIR.0000000000001123
-
Centers for Disease Control and Prevention. Stroke facts. Updated October 24, 2024. Accessed March 20, 2025. https://www.cdc.gov/stroke/data-research/facts-stats/index.html
Centers for Disease Control and Prevention. Stroke facts. Updated October 24, 2024. Accessed March 20, 2025. https://www.cdc.gov/stroke/data-research/facts-stats/index.html
-
Winstein CJ, Stein J, Arena R, et al. Guidelines for adult stroke rehabilitation and recovery: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2016;47(6):e98-e169. doi:10.1161/STR.0000000000000098
Winstein CJ, Stein J, Arena R, et al. Guidelines for adult stroke rehabilitation and recovery: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2016;47(6):e98-e169. doi:10.1161/STR.0000000000000098
-
Saver JL. Time is brain—quantified. Stroke. 2006;37(1):263-266. doi:10.1161/01.STR.0000196957.55928.ab
Saver JL. Time is brain—quantified. Stroke. 2006;37(1):263-266. doi:10.1161/01.STR.0000196957.55928.ab
-
El-Koussy M, Schroth G, Brekenfeld C, Arnold M. Imaging of acute ischemic stroke. Eur Neurol. 2014;72(5-6):309-316. doi:10.1159/000362719
El-Koussy M, Schroth G, Brekenfeld C, Arnold M. Imaging of acute ischemic stroke. Eur Neurol. 2014;72(5-6):309-316. doi:10.1159/000362719
-
Heiss WD. The ischemic penumbra: correlates in imaging and implications for treatment of ischemic stroke. The Johann Jacob Wepfer Award 2011. Cerebrovasc Dis. 2011;32(4):307-320. doi:10.1159/000330462
Heiss WD. The ischemic penumbra: correlates in imaging and implications for treatment of ischemic stroke. The Johann Jacob Wepfer Award 2011. Cerebrovasc Dis. 2011;32(4):307-320. doi:10.1159/000330462
-
Powers WJ, Rabinstein AA, Ackerson T, et al. Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2019;50(12):e344-e418. doi:10.1161/STR.0000000000000211
Powers WJ, Rabinstein AA, Ackerson T, et al. Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2019;50(12):e344-e418. doi:10.1161/STR.0000000000000211
-
Arch AE, Weisman DC, Coca S, Nystrom KV, Wira CR III, Schindler JL. Missed ischemic stroke diagnosis in the emergency department by emergency medicine and neurology services [published correction appears in Stroke. 2016 Mar;47(3):e59. doi:10.1161/STR.0000000000000099]. Stroke. 2016;47(3):668-673. doi:10.1161/STROKEAHA.115.010613
Arch AE, Weisman DC, Coca S, Nystrom KV, Wira CR III, Schindler JL. Missed ischemic stroke diagnosis in the emergency department by emergency medicine and neurology services [published correction appears in Stroke. 2016 Mar;47(3):e59. doi:10.1161/STR.0000000000000099]. Stroke. 2016;47(3):668-673. doi:10.1161/STROKEAHA.115.010613
-
Demaerschalk BM, Kleindorfer DO, Adeoye OM, et al. Scientific rationale for the inclusion and exclusion criteria for intravenous alteplase in acute ischemic stroke: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2016;47(2):581-641. doi:10.1161/STR.0000000000000086
Demaerschalk BM, Kleindorfer DO, Adeoye OM, et al. Scientific rationale for the inclusion and exclusion criteria for intravenous alteplase in acute ischemic stroke: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2016;47(2):581-641. doi:10.1161/STR.0000000000000086
-
Menon BK, Buck BH, Singh N, et al. Intravenous tenecteplase compared with alteplase for acute ischaemic stroke in Canada (AcT): a pragmatic, multicentre, open-label, registry-linked, randomised, controlled, non-inferiority trial. Lancet. 2022;400(10347):161-169. doi:10.1016/S0140-6736(22)01054-6
Menon BK, Buck BH, Singh N, et al. Intravenous tenecteplase compared with alteplase for acute ischaemic stroke in Canada (AcT): a pragmatic, multicentre, open-label, registry-linked, randomised, controlled, non-inferiority trial. Lancet. 2022;400(10347):161-169. doi:10.1016/S0140-6736(22)01054-6
-
Cannon CP, McCabe CH, Gibson CM, et al. TNK-tissue plasminogen activator in acute myocardial infarction. Results of the Thrombolysis in Myocardial Infarction (TIMI) 10A dose-ranging trial. Circulation. 1997;95(2):351-356. doi:10.1161/01.cir.95.2.351
Cannon CP, McCabe CH, Gibson CM, et al. TNK-tissue plasminogen activator in acute myocardial infarction. Results of the Thrombolysis in Myocardial Infarction (TIMI) 10A dose-ranging trial. Circulation. 1997;95(2):351-356. doi:10.1161/01.cir.95.2.351
-
Keyt BA, Paoni NF, Refino CJ, et al. A faster-acting and more potent form of tissue plasminogen activator. Proc Natl Acad Sci U S A. 1994;91(9):3670-3674. doi:10.1073/pnas.91.9.3670
Keyt BA, Paoni NF, Refino CJ, et al. A faster-acting and more potent form of tissue plasminogen activator. Proc Natl Acad Sci U S A. 1994;91(9):3670-3674. doi:10.1073/pnas.91.9.3670
-
Bennett WF, Paoni NF, Keyt BA, et al. High resolution analysis of functional determinants on human tissue-type plasminogen activator. J Biol Chem. 1991;266(8):5191-5201.
Bennett WF, Paoni NF, Keyt BA, et al. High resolution analysis of functional determinants on human tissue-type plasminogen activator. J Biol Chem. 1991;266(8):5191-5201.
-
Warach SJ, Dula AN, Milling TJ, et al. Prospective observational cohort study of tenecteplase versus alteplase in routine clinical practice. Stroke. 2022;53(12):3583-3593. doi:10.1161/STROKEAHA.122.038950
Warach SJ, Dula AN, Milling TJ, et al. Prospective observational cohort study of tenecteplase versus alteplase in routine clinical practice. Stroke. 2022;53(12):3583-3593. doi:10.1161/STROKEAHA.122.038950
-
Campbell BCV, Mitchell PJ, Churilov L, et al. Tenecteplase versus alteplase before thrombectomy for ischemic stroke. N Engl J Med. 2018;378(17):1573-1582. doi:10.1056/NEJMoa1716405.
Campbell BCV, Mitchell PJ, Churilov L, et al. Tenecteplase versus alteplase before thrombectomy for ischemic stroke. N Engl J Med. 2018;378(17):1573-1582. doi:10.1056/NEJMoa1716405.
-
Hendrix P, Gross BA, Allahdadian S, et al. Tenecteplase versus alteplase before stroke thrombectomy: outcomes after system-wide transitions in Pennsylvania. J Neurol. 2024;271(8):5637-5641. doi:10.1007/s00415-024-12530-x
Hendrix P, Gross BA, Allahdadian S, et al. Tenecteplase versus alteplase before stroke thrombectomy: outcomes after system-wide transitions in Pennsylvania. J Neurol. 2024;271(8):5637-5641. doi:10.1007/s00415-024-12530-x
-
Seners P, Wouters A, Ter Schiphorst A, et al. Arterial recanalization during interhospital transfer for thrombectomy. Stroke. 2024;55(6):1525-1534. doi:10.1161/STROKEAHA.124.046694
Seners P, Wouters A, Ter Schiphorst A, et al. Arterial recanalization during interhospital transfer for thrombectomy. Stroke. 2024;55(6):1525-1534. doi:10.1161/STROKEAHA.124.046694
-
-
